Interplay of traumatic birth experiences and postnatal depression in Pakistani women
The birth of a child is an exciting yet potentially overwhelming experience, often accompanied by feelings of burden, worry, sadness, and self-doubt. Postnatal depression (PND), a persistent depressive disorder following childbirth, ranges from mild sadness to severe depression and often co-occurs with anxiety. If untreated, PND can last for years. Also referred to as postpartum depression (PPD), up to 40% of PND cases begin during pregnancy1.
Key indicators of PND include severe sadness, loneliness, mood swings, hopelessness, fatigue, guilt, loss of appetite, and frequent crying spells2. According to the International Classification of Diseases (ICD-10), postpartum depression occurs within the first 42 days after childbirth3,4. If left untreated, it adversely affects maternal relationships, physical health, childcare, and professional functioning, and is associated with substance abuse and breastfeeding difficulties5.
PND is a major public health concern, affecting up to 17% of healthy mothers globally, though prevalence varies widely6,7. In high-income countries such as Singapore, the Netherlands, and Switzerland, rates range from 3 to 11%, whereas in low- and middle-income countries (LMICs) like Pakistan, India, and Nepal, rates are much higher due to socioeconomic disparities, maternal/infant mortality, and women’s workload6. Studies in Pakistan report prevalence rates from 28% to 63%, with cesarean delivery linked to higher risk8,9.
Despite the higher vulnerability of women in LMICs, research on PND remains limited. Understanding its predictors and consequences within diverse sociocultural contexts is essential for developing effective interventions. Although demographic, social, and obstetric factors have been identified as contributors, they remain underexplored in LMIC settings.
Although the exact etiology of PND remains unclear, studies have identified multiple risk factors, including low educational attainment10, prior psychiatric history, perinatal stress, insufficient partner or family support, relationship conflicts, domestic violence, and major life stressors such as bereavement or separation11,12. Economic hardships and limited access to healthcare also exacerbate the risk13. Additionally, maternal characteristics such as age, parenting confidence, and socioeconomic status—often inferred through education level—significantly influence PND risk. For example, women with higher education are less likely to experience PND10,14. In Pakistan, PND is more prevalent among young, low-income, less-educated housewives living in extended families15.
Obstetric complications and traumatic birth experiences are also significant contributors to PND. Severe obstetric complications have been associated with increased risk for PND and poorer physical health15,16. Negative experiences, such as obstetric violence and invasive medical interventions, further exacerbate the risk17,18,19. Obstetric violence includes mistreatment, negligence, and human rights violations during childbirth20. Traumatic childbirth experiences often lead to increased PND risk, future fear of childbirth, and preferences for cesarean delivery21,22.
Satisfaction with childbirth is another critical obstetric factor that determines PND. Factors influencing satisfaction include personal expectations, support during delivery, quality of caregiver-patient relationships, and participation in decision-making23. Studies consistently report an inverse relationship between birth satisfaction and PND risk24,25. For example, Urbanová et al.26 found that lower childbirth satisfaction significantly predicted higher PND risk, even after controlling for sociodemographic and clinical variables.
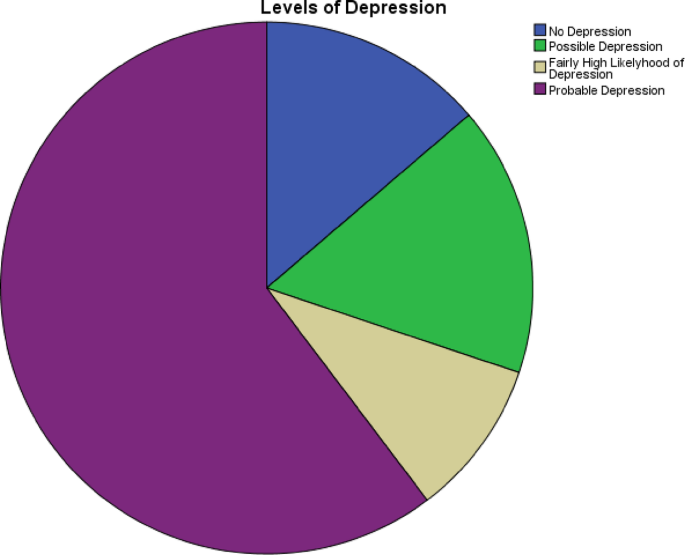
Postnatal depression is a pressing public health concern in Pakistan, with prevalence rates ranging from 28% to 63%. These figures are alarmingly higher than those reported in many developed countries, reflecting a significant burden on maternal and infant health. Despite its prevalence and adverse outcomes—including impaired maternal well-being, negative infant development, and strained family dynamics—PND remains an underexplored area in Pakistan. Most of the existing research has been conducted in Western contexts, where sociocultural, economic, and healthcare conditions differ significantly from those in low- and middle-income countries (LMICs) like Pakistan. The lack of indigenous studies on PND limits the understanding of its prevalence, underlying factors, and cultural nuances in Pakistan. In particular, obstetric factors such as delivery method, birth complications, perceived birth trauma, and satisfaction with childbirth, which have been shown to influence PND risk in other contexts, are understudied in the Pakistani population. Pakistani women represent a unique population for studying birth satisfaction and postnatal depression due to the country’s distinct sociocultural context, family structures, and maternal care practices. Traditional gender roles, limited mental health awareness, and varying access to maternal healthcare services influence women’s childbirth experiences and emotional well-being in ways that differ from Western populations. Understanding these factors within the Pakistani context is essential for developing a culturally sensitive interventions and policies to support maternal mental health.
Although international research has extensively explored birth satisfaction and postnatal depression, there is limited empirical evidence from Pakistan addressing how healthcare practices, and other negative birth experiences lead to PND in postnatal women. Existing studies in the region often focus on medical outcomes rather than women’s psychological and emotional well-being. Moreover, few studies have simultaneously examined birth satisfaction and postnatal depression using standardized measures within the Pakistani context. This gap highlights the need for context-specific research to understand the psychological dimensions of childbirth. The current study addresses these gaps by examining the relationship between obstetric factors and PND symptoms during the postpartum period (42–84 days). By focusing on the Pakistani context, this research will contribute to the take evidence-based, culturally sensitive preventive and curative measures for identifying and addressing PND in vulnerable women in Pakistan.
Hypotheses
Following hypotheses were tested in the study:
H1:
Delivery method, mother birth complications, infant birth complications, birth trauma perception, previous birth trauma, and birth satisfaction significantly correlate with the post-natal depression in postnatal Pakistani women;
H2:
Delivery method, mother birth complications, infant birth complications, birth trauma perception, previous birth trauma, and birth satisfaction significantly predict post-natal depression in Pakistani women after controlling demographic variables (viz., age, income groups, area, and education).
link